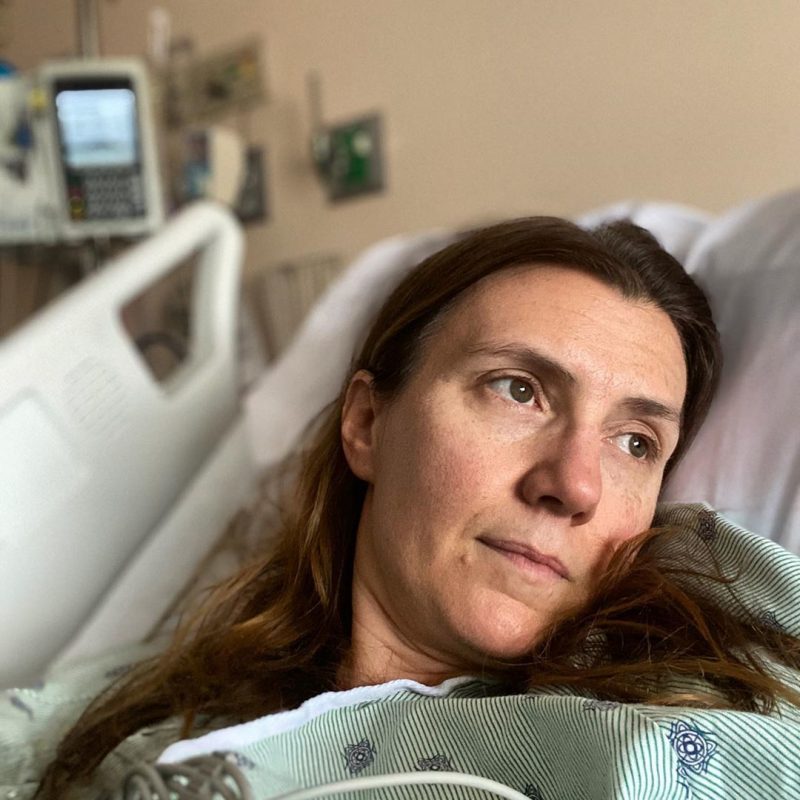
When Cara Ober, the editor of local arts magazine BmoreArt, went to St. Joseph’s Hospital Medical Center for a chest X-ray last Sunday, she never thought she’d be admitted. Instead, she thought she’d get a more clear diagnosis for her persistent chest congestion, fever, body aches, and dizziness—and, hopefully, the Golden Ticket of healthcare these days: a test for COVID-19.
Instead, they told her she had bad pneumonia and needed to be hospitalized immediately. She eventually got that COVID-19 test, although she’s still awaiting the result.
She’s home now, quarantined in her room with her rescue chihuahua, Mr. Big. She says she’s not sure if she’ll ever see the result of her test. (“My doctor said don’t hold your breath—ha ha.”) A friend of hers, who works for the CDC in a different state, described the state of affairs as a “sh*tshow,” and said that many tests have been lost.
When asked on a scale from 1-10 how sure she is that she had coronavirus, Ober doesn’t hesitate: “Ten.”
Thankfully, she’s feeling much better. She still gets headaches in the afternoon, still has a little tightness in her chest. But no fever. Although she was quite sick, the hospital was never forced to put her on a ventilator.
The hardest part, of course, has been staying separate from her husband and nine-year-old son, Leo.
Coincidentally, Leo is reading a series of fictionalized accounts of kids who survived famous disasters—the volcanoes of Pompei, the bombs of Hiroshima—titled I Survived.
“I just said, ‘Kiddo, you can write your own I Survived after this,’” she says.
In a way, Ober has written such an account herself. She published a powerful personal essay about her ordeal with the virus in BmoreArt.
She said writing it was cathartic. But it had a larger purpose, too: For Ober, it’s crucial that people read as much as they can about the virus because she feels like the information out there is insufficient, and not always accurate.
“For me, the most important thing is that people are educating themselves,” she says. “If I thought there was better information out there, I wouldn’t feel so much urgency.”
Her essay is reprinted here, in full, with her permission.
Fever Dream: Symptoms, But No COVID-19 Tests and No Results
It took eight days of coronavirus symptoms and a trip to the ER to get a test.
By Cara Ober | Published March 28, 2020 at BmoreArt.com
I wake up with a fever of 102 in the middle of a global pandemic. It doesn’t take a genius to figure out that I should immediately be tested for coronavirus in order to help stop the spread of disease, but this doesn’t happen. After two weeks of fevers, pneumonia, and hospitalization, I am finally tested, but receive no results. At this point, I don’t need a test to tell me that I have COVID-19 and my experience suggests that thousands of very sick people are in the same predicament, suffering from a brutal viral infection with very few medical resources, and left out of official headcounts. We need more information, more data, more accessibility to testing and medical resources in order to protect ourselves and others from this deadly illness and it’s not happening.
My initial symptoms are insignificant. My head feels warm and buzzy. Is this a hot flash? Am I sick? I’m fine. I haven’t travelled overseas. I haven’t come into contact with anyone who has tested positive for coronavirus. Maybe I’m just having global pandemic anxiety that is inducing a physical reaction? Maryland has just closed schools and encouraged people to stay at home and social distance, and my son and I take walks around the neighborhood with our dogs.
On Sunday, March 15 I feel worse, but not terrible. I conduct a phone interview with an artist friend living in Italy, trying to understand what may be coming to the US in a week or two, and we publish it the next day as a dire warning. My body feels off, but not that bad. I suspect a fever but none of our thermometers are working. I spend an hour combing through our bathroom closet, throwing away dozens of expired medications. My husband orders batteries for our digital thermometer from Amazon, because there were no thermometers in stock at any of the drug stores near my house.
On Monday I wake with a fever of 102. The batteries have arrived. I shiver, sweat, and ache in every bone and joint. I have no appetite, no sense of taste or smell. I am so tired I stay in bed all day. The only escape from this misery is sleep. I call my primary care physician, who is not doing in-person appointments and has switched his practice to phone triage to accommodate more patients. He asks me if I have been out of the country within two weeks (I hadn’t) and if I had come into contact with anyone who had tested positive (nope). He asks if I have a sore throat, cough, or shortness of breath, the primary symptoms of coronavirus besides a high fever (I do not). I ask if I can have a COVID-19 test, in order to protect my family and those I have been in contact with and am shocked to learn that I do not qualify.
I am flummoxed. In the middle of an exponentially expanding outbreak, when thousands are dying daily, and the only tool we have to track and contain this virus is a test, a person with a 102-degree fever does not qualify? What kind of absurd, dark comedy am I living in? My doctor explains that unless I were elderly with symptoms or could prove contact with someone who tested positive, I cannot get a test. My instructions are to stay at home, hydrate, take Advil or Tylenol for the fever, and rest. I agree to call my doctor if my current symptoms worsen or if I develop respiratory symptoms, but there is no discussion of the possible progression of symptoms experienced by those with COVID-19, the fact that symptoms change every few days, or what kinds of medicine I should take should those symptoms evolve.
Feeling terrible in bed, Day 3 of sickness, March 18, 2020.
Mr. Big, Ober’s dog and constant companion in bed the first week.
My husband moves into the guest room and forces me to drink Pedialyte several times a day, which is disgusting but I can’t taste it anyway. I sleep for several days, rarely getting up, and when I’m awake, I read articles that infuriate and terrify me about COVID-19 symptoms and our government’s lack of a coherent response. I think I’m getting worse, I tell my husband. He tells me to stop reading the news.
What would have been helpful to know in the beginning is that COVID-19 symptoms fluctuate wildly, that there are periods where I feel almost normal and want to eat actual food or spend time out of bed, potentially infecting my family members. Over and over I think, finally, the worst is over, only to have the fever return, like Charlie Brown with that damn football.
My husband and son have no symptoms, so we assume that I have the regular flu, an unfortunate coincidence, since both of them had gotten flu shots and I didn’t. It seems I am on the mend on Wednesday, March 18, after a nasty few days. That day I read an entire novel (The Dutch House by Ann Patchett) and then watch a movie with my family in the evening, sitting a few feet away from them. But that night, I feel a pinching in my lungs, a dry cough when I try to inhale. It was suddenly as if someone had tightened a belt around my lungs and I can’t take a full breath.
I wake up at 3 a.m. with a stabbing pain in the left side of my chest. Is it my heart? Are my lungs collapsing? I can feel the steam rolling off me and I’m lying in a puddle of sweat. I lie in bed for a while longer, wondering if I’m dying from COVID-19, and worse, if I have infected the people I love most. I sit up and feel a sharp intake of breath, a sickening but familiar feeling. I cannot accommodate my own breath, and a fit of coughing ensues. I pull myself out of bed, fill up a glass of water and take two Tylenol to curb the fever. I try to do all this quietly and in the dark because I don’t want to wake my husband and son, sleeping in separate bedrooms.
“In the middle of an exponentially expanding outbreak, when thousands are dying daily, and the only tool we have to track and contain this virus is a test, a person with a 102-degree fever does not qualify? What kind of absurd, dark comedy am I living in?”
At this point, it is just the beginning, but I don’t yet realize it. It has been several long days for me with coronavirus symptoms and I’m living every second in a bizarre purgatory of fever, chills, guilt, fear, and the frustration of not knowing if I have it or not.
I wake up on Thursday to a flurry of texts from friends and colleagues. Am I better yet? How am I doing? Have I gotten tested? Have I talked to my doctor? Have I seen the latest idiotic thing our president has said? Do I still have a fever?
It feels like a personal failure to tell all of them that, no, I am not better and yes, I still have a fever. American capitalism has trained us to think we have control over our lives and livelihood to the point where even serious health issues are seen as a mind-over-matter problem to be solved quickly, and I think the coronavirus pandemic has proven this as a complete fantasy. We are not in control and we are not prepared and the US healthcare system—or industry, as it actually is here (there are shareholders and payoffs, are there not?)—is not set up to care for people when they need it the most.
I wait until Thursday at nine to call my doctor the minute the office opens. My sickness has gone respiratory, I tell him, thinking that now I will finally be tested. I have shortness of breath and a cough in addition to the fever, which shoots up every time the Advil wears off. I am weak with no appetite, and no sense of smell although my nose isn’t clogged. I am shocked that I still do not qualify for a COVID-19 test. It has been five days with fever and every single symptom except a sore throat. My doctor explains that as long as I’m not wheezing or feeling like I can’t get enough oxygen, I do not qualify for a test.
On Friday evening, I become more and more terrified by my shallow and rapid breathing. I had taken a break from reading the news, but found a helpful triage site made by a group of doctors that suggested those suffering from coronavirus symptoms take an expectorant and decongestant to help with breathing. Within a few minutes of drinking the most disgusting battery acid pink liquid, my breathing calms. I still can’t take a deep breath, but it’s better. Whew. Reading about all those Italians suffocating in their own collapsed lungs does not help my mental state, but in this case the fear is warranted. I continue to take an expectorant and decongestant every four hours, and I can tell as soon as it leaves my system because my breathing becomes ragged again.
On Sunday, eight full days since I first fell ill, I awake to a splitting headache and feel a shortness of breath coupled with a new dizziness. Am I getting worse? Or is my body extra tired from fighting this thing? My doctor’s office is closed so I call and leave him a message.
My husband and son are still asymptomatic. For more than a week, I have been a non-parent, almost a non-human in my own home. Every day they take long walks with the dogs, ride bikes, read books, play video games, watch movies. My son understands that he cannot play with the neighborhood kids and hasn’t complained about it, so I appreciate that and wonder if he is secretly terrified. I worry that the two of them will get sick, and this fear is worse than anything.
I go back and forth about my symptoms, waiting for a call back. Should I harass my doctor to get the test so that I have irrefutable proof that I have it? Is it my duty as a citizen to be counted and added to the numbers so that doctors can do proper research on this pandemic in my community? If I can get approved for a test, do I have the strength to drive myself to a parking garage to wait in line for hours for a nose swab? And what do I do if my lungs get worse? Should I go to an urgent care health clinic or to the hospital and risk exposure to all kinds of germs? How sick is sick enough to go? How the hell is staying at home with zero medical intervention the best medical care one can get during a global health crisis? I remind myself that I am one of the lucky ones who can breathe and whose family is healthy, and I just need to focus on getting better, little by little. I calm down.
I’m shocked to get a call back from my doctor on Sunday midday. He is clear and decisive. It’s time to go immediately to the emergency room and get a chest X-ray. He says that the length of time that I have had worsening symptoms, the fever and the respiratory issues, sound like COVID-19 and I need care. I go back and forth about this in my mind, imagining a hospital scene of carnage, germs, piles of wheezing sick people, and a lack of medical supplies, and then I tell my husband I’m going. I put on a painter’s face mask from Home Depot, which feels ridiculous, but I know it’s a protective gesture to those who work at the hospital.
It has been a week since I last left my house, a week since I’ve driven my car. St. Joseph Medical Center is the closest hospital to my house, and when I get there the ER parking lot is weirdly empty. I park, hop out, and almost turn back to leave after I read the sign in the window: “At this time, we do not have COVID-19 testing available for all patients.” Is it closed? There is a sad looking plastic tent and some caution tape in front of the revolving door. Oh wait. There’s a side door. I press the button with my elbow, trying not to touch anything.
Inside, two receptionists are wearing masks and zero patients are in the waiting room. “My doctor told me to come,” I wheeze. “He wants me to get a chest X-ray for pneumonia.” They take my information and I wait, breathing in my industrial mask, before I am brought back into the ER. My quickly identify me as a COVID-19 risk and everyone who visits me is encased in plastic masks and garments. They take vials of my blood and the X-ray tech comes to me and takes a photo of my lungs in my room with the door closed. They ask me to keep my mask on to protect them.
Within a few minutes, the ER doctor is telling me I have pneumonia, a common effect of COVID-19. He says my lungs look “very bad.” He says I am midway between the early and late stages of coronavirus symptoms, with the third being a total collapse of the lungs, which requires immediate action in order to prevent. He says they want to aggressively treat me with IV antibiotics, Azithromycin, for viral pneumonia, and asks if I want to be part of a clinical trial for use of Plaquenil, an anti-malaria drug that may or may not help with COVID-19 that Trump was touting as “very promising” on the news. At this point, I’ll take anything, although studies have now shown that the drug has no impact on coronavirus treatment.
The doctor explains that he wants to give me the COVID-19 test, but he is only allowed to if I fail two other tests first, so we begin. They take more of my blood, insert an IV into one arm, and do nose swabs. After 45 minutes, they tell me my flu test is negative. They give me the second test, a viral panel, and an hour later I am negative for this too. They then give me the COVID-19 test and tell me I should have the results in 48 hours. The doctor says he wants to admit me to the hospital, that I’m very sick and they need to keep a close watch on my lungs.
A nurse encased in plastic wheels me upstairs. They take even more blood, hook me up to a bag of fluid and antibiotics, and, mostly, let me sleep. I made the huge mistake of having them put the IV in my right arm, so every time I text anyone my vitals monitor beeps angrily in protest, but I soon learn how to reset it.
My room is clean and quiet, and I appreciate the rest. It is a relief to not feel guilty every time my son asks for a drink or some food or has a question, to not have to explain why he has to ask his father instead of me and keep a distance. It’s a comfort to know that professionals are monitoring my heart and lungs and I’m not going to die alone in the middle of the night. For three days, I nap and eat hospital food. I watch a little TV, but not much. I am pumped full of medications and fluids. I make phone calls to all the people who are worried about me, and I sleep. I’m not bored. I’m not lonely. I’m tired, and I realize that, for the first time in over a week, I feel safe.
I have a respiratory specialist who visits me four times a day to give me an inhaler and test my lung functioning. I have a doctor who visits once a day, under a layer of plastic, and he gives me his cell number. He texts me from Eddie’s the next day and offers to bring me snacks, which is endearing beyond any normal scale of bedside manner. I have nurses who are so kind, so professional, and so generous that it brings me to tears to realize they are risking their lives every time they enter my room. Several of them tell me about the small children they have at home and how they attempt to mini-quarantine after each day at work surrounded by illness and germs. It breaks my heart to wonder how many of them will get sick in the coming weeks, just from showing up and doing their jobs well.
Left: My lungs. They’re supposed to be all black, which is the oxygen but they are full of whispy white stuff, the pneumonia. Right: my IV and bar code.
Anyone who enters my room is encased in a yellow plastic gown, plastic face shield, and respiratory mask. Their outer layer is shed every single time they leave my room. By the end of my stay, there are two large trash cans overflowing with these tainted outer layers. They cannot take my germs with them into the rest of the hospital. I am contagious, potentially deadly to them, to other patients, and to those they love.
After three days my breathing begins to improve, and my doctor and I discuss an exit strategy. He tells me there are about 30 other patients in the hospital waiting for COVID-19 test results and that the federal testing program says it will take 6 to 8 business days to get the results back. My test has been sent to a CDC testing facility in Pennsylvania, and then to New York. He explains that there is a very high rate of false negative results with these tests in particular, but almost no false positives, and that he has learned this from conversations with other health professionals across this country.
What this means is there are a lot more people with coronavirus than what is being reported, even among those who meet the restricted qualifications to be tested. I realize he is preparing me for a false negative test result, even though from my symptoms it is clear that I have COVID-19. He tells me I am potentially contagious for two weeks after my last fever, and instructs me to behave as though I have received a positive test result no matter what.
On Wednesday, March 24 I am discharged from the hospital. It’s cold and drizzly and surreal as I walk to my car, still sitting in the ER parking lot, which is still mostly empty. I look forward to sleeping in my own bed, and my husband and I have hatched a plan for me to quarantine in our bedroom with the dog, and for him and my son to essentially live their lives as far away from me as they can in the same house for the next two weeks.
I am still exhausted and have no appetite. I am getting migraine-level headaches every afternoon, but I can inhale completely, with just a small amount of coughing. My pneumonia is on the mend. This time, I know better than to expect a speedy recovery. COVID-19 lingers and changes, flickers away and returns with unexpected force. It is brutal and almost calculating, and this fluctuation in symptoms and false sense of improvement encourages its spread.
“At this point, if I receive a negative test, it really doesn’t matter. It’s not as if I would suddenly open up my doors and hug my child or make out with my husband or go grocery shopping. Can you imagine a single human acting this way after going through all of this?“F
Two days later, people want to know if I am better yet and are shocked that I still haven’t gotten my test results. I’m better, but I’m not well, I respond. No results yet, I say. My regular doctor calls me to check in and tells me he was told 8 to 10 business days for my results. The CDC is experiencing a backlog and can’t keep up with the testing and he confirms that there is a high number of false negative results with these particular tests made in the USA. I am still experiencing extreme fatigue, migraine-level headaches that show up each afternoon, but no fever. And I can breathe again.
Back at home from the hospital with Mr. Big in bed, Day 11 of being sick, March 26, 2020
At this point, if I receive a negative test, it really doesn’t matter. It’s not as if I would suddenly open up my doors and hug my child or make out with my husband or go grocery shopping. Can you imagine a single human acting this way after going through all of this? No. It’s clear that I’m not OK. It would be irresponsible to everyone I know and love, and disrespectful to all those healthcare workers at the hospital, to behave in any way that does not reflect that I have COVID-19.
If my test is negative, I know that my suffering will not be officially counted, that my case will not be added to the growing statistics against a federal government completely unprepared and uneducated in its response to this pandemic. What scares me most is realizing that there are so many people in this region suffering from similar symptoms, that some are dying, and that most of them are not being tested.
It makes absolutely no scientific or ethical sense to deny coronavirus tests to those with symptoms, any symptoms, but this is our current reality: It is very difficult to qualify for this test and takes up to two weeks to get a result. This means the numbers currently being reported are from illnesses from two weeks ago and drastically lower than actual cases.
After I posted an announcement on social media, so many people have reached out to me who are suffering from fevers, coughs, and flu symptoms in the middle of a public health crisis so serious it has shut down the entire world’s economy—but there are no tests available for these people.
It is insane that the US government knew about the coming crisis in January, had all the research available from China, and did nothing to prepare except to spread disinformation. It’s offensive to know that we were offered working test kits from the World Health Organization and our government turned them down, and instead made their own faulty kits.
It’s absurd that Americans believe that we have the best healthcare system in the world, and that capitalism mandates that our hospitals and pharmaceutical companies make a profit from the sick. It’s not economically feasible to adequately prepare for a pandemic, and yet here we are. Our country isn’t even comprehensively tracking known cases and making it available to researchers and health professionals, so how do we have any sense of how to protect the spread of this virus? It’s time to ask ourselves if this is the kind of country we want to continue to live in, where celebrities and asymptomatic NBA athletes receive medical services, while 99.9 percent of regular people cannot access them during a global health crisis.
When I get my test results, I will announce it publicly, but the truth is they don’t matter. My experience is proof that our healthcare system does not function in a responsible way and that people are dying as a result. It is dangerous for anyone and everyone to go outside. We are not testing even a fraction of the people who should be tested for COVID-19 in order to have accurate data and, of those tested, there are a high number of false negative results. This means we have potentially thousands more individuals who have coronavirus in our region alone, and our health response is inadequate and ill-informed, with individual hospitals, doctors, and healthcare workers bearing the brunt of this crisis. These people are my heroes.
I am on the mend, although I am fearful that my symptoms may return, based on what I’m hearing from others with similar symptoms. I received excellent care from St. Joseph’s hospital and from my regular doctor who is doing the best he can within a dysfunctional nightmare.
We all have an opportunity to make our voices heard and to demand that our government and the media, which continue to spread misinformation via White House briefings, take our demands seriously. We can write. We can tweet. We can choose not to watch those bogus performances. We can stay home and wash our damn hands. We can vote in the primaries and in November. And we can support the local businesses and organizations we love now so that they still exist after this crisis is over.
No one is coming to save us, especially not the federal government. We have got to educate and save ourselves, to support one another, to take our own health concerns seriously, and to demand a health care system that serves and protects everyone.
Read more on Ober’s experience, and her thoughts on the shared sense of isolation we’re all dealing with, here.
