Unsung Heroes Of Health Care
Our second annual Excellence in Nursing awards honor some of Baltimore’s best RNs.
By Ken Iglehart, Rebecca Kirkman, and Christianna McCausland | Photography by David Colwell.

Okay, We Have To Ask:
In health care, why do physicians get all the credit?
The answer probably has a lot to do with a seriously outdated perception of the role played by another group of medical professionals: registered nurses. They’re the thin white line of health care that, in the past 20 years or so, has taken on a multitude of new responsibilities once handled by doctors, in sickness and in health. The other question we should be asking? “Is there a nurse in the house?”
You’d be hard-pressed to find a region with more great nurses than metro Baltimore, and our job in Baltimore’s second annual Excellence in Nursing survey was to find some of those stars.
To arrive at the results, the unveiling of which coincides with National Nurses Week in May, we solicited nominations from peers, supervisors, and patients of registered nurses—both in and out of hospitals—who represent the finest in their field, and we received an overwhelming response. And in our accompanying story, “All in a Day’s Work,” we look at the typical harried day of a critical-care nurse at a hospital that gets plenty of ER action.
There were 17 nursing specialties for which we accepted nominations in a process that took nine months. Then the hard part began: picking the finalists. For that, we relied on the Maryland Nurses Association and major local hospitals to help us recruit an impressive panel of highly experienced RN advisers, who divvied up the specialties and pored over the hundreds of nominations to arrive at our winners. Congratulations to all 55 of them.
Meet Our Survey Advisors
We offer a tip of the nurse’s cap to our seven registered-nurse advisers, who lent their time, considerable expertise, and reputations to the survey process. Our advisers—several of whom re-upped for a second year in this role—are not eligible to be on the list of winners in the year they serve.

Linda K. Cook
Linda K. Cook Ph.D., RN, CCRN, CCNS, ACNP-BC, is an assistant professor at the University of Maryland School of Nursing. Dr. Cook has nearly 40 years of nursing experience, mainly in critical care and education. She is also the treasurer of the Maryland Nurses Association. Dr. Cook currently resides in Lanham.

D. Paxson Barker
D. Paxson Barker, Ph.D., MS, RN, has been a registered nurse for 43 years, most of that as a cardiovascular nurse specialist, and now serves as a public-health nurse specializing in environmental and occupational health. She currently teaches courses in an online format for graduate and undergraduate nursing students, including community/global health, population health, and dissertation completion.

Kim Bushnell
Dr. Kim Bushnell, DNP, MSN, RN, is the vice president for patient-care services and chief nursing officer at Mercy Medical Center. Her clinical background includes trauma and emergency, critical care, and flight nursing.Bushnell received her BSN from George Mason University in Virginia,
her MSN from The Catholic University in Washington, D.C., and her DNP from The Johns Hopkins University School of Nursing.

Jenny Bowie
Jenny Bowie, RN, BSN, MBA, is the vice president of patient-care services and chief nurse executive at Mt. Washington Pediatric Hospital, providing strategic oversight for nursing, professional practice, respiratory therapy, pharmacy, infection prevention, and collaborative care. Bowie previously worked in various academic and community
health care settings.

Joann M. Oliver
Joann M. Oliver, MNEd, RN, CNE, CBIS, received her BSN from Penn State and her master’s in nursing education degree from the University of Pittsburgh. A certified nurse educator and a certified brain-injury specialist, she teaches at Anne Arundel Community College, and is the recent past vice president of the Maryland Nurses Association.

Lynn Marie Bullock
Lynn Marie Bullock, DNP, RN, NE-BC, is the administrative director of the nursing professional practice at Greater Baltimore Medical Center. Bullock earned her bachelor’s of nursing degree from Syracuse University, a master’s of nursing degree and certificate in nursing education from Towson University, and a doctor of nursing practice degree from The Johns Hopkins University School of Nursing.

Idriz Limaj
Idriz Limaj, LNHA, RN, is the chief operating officer of Levindale Hebrew Geriatric Center and Hospital and the post-acute division at LifeBridge Health. The post-acute services Limaj oversees include long-term care, behavioral health, chronic hospital services, and skilled nursing-home care, as well as outpatient day-treatment programs and adult-day services. The division is located at Northwest Hospital and Levindale.

Erynn Bossom
Nurse Manager, Neuro Telemetry Unit
Saint Agnes Hospital
What does your unit do? We focus on the care of the neurological population and specialize in stroke care.
What inspired you to get into the field? I come from a long line of nurses and have always been driven to help others.
How has nursing evolved during your career? The shift to evidence-based practice has allowed nurses to achieve the best possible outcomes based on research.
What is the most important attribute for a nurse? The most valuable qualities for our nurses are their compassion and their keen assessment skills, which allow them to identify the smallest of changes and act appropriately.
What’s the greatest reward in being a nurse? I’d say it’s watching the new graduate nurses grow and develop. But my favorite moment was when a nurse came to me on his last day to thank me for helping him on his journey. He had struggled significantly as a new graduate, but is now starting the nurse anesthetist program. I couldn’t be more pleased for him.
What’s your biggest challenge? Like many nurses, it’s maintaining a healthy work-life balance. I love both so much and work diligently to maintain that balance.
What other kudos have you received for your work? I’ve been nominated for many nurse-excellence awards in the category of performance improvement.
What’s your best advice for those getting into the field? Never stop learning and always ask questions.

Phyllis Hawkins
Heart care unit/subacute rehabilitation
Lifebridge Health Northwest Hospital
How has nursing evolved? There are many more demands put on nurses these days, but I also think people are often sicker than they were, perhaps because of unhealthy lifestyles and diets. There’s also a lot more work keeping up with new technology, new regulations, and new data-recording systems.
What’s the most critical quality for a nurse in your specialty? I think just having the compassion it takes to really do nursing, and understanding that it’s not just a 9-to-5 thing—you have to really want to care for people.
What’s your biggest challenge? Not having enough time in the day to get everything done.
What do you consider the profession’s greatest rewards? When you see someone get well, and you know you’ve made a difference in someone’s life, that’s the best feeling ever.
What advice do you give to new nurses? Sometimes people come into nursing not understanding that they may sometimes have to do it all: They may have to empty a bedpan, or clean up the bed if someone vomits. You better be ready to wear many different hats, but it’s such a rewarding profession.
What would you have done as a career if you hadn’t been a nurse? I think I would have been a schoolteacher. I like small kids, and would have loved to teach kindergarten to first grade.

Joan Geckle
Staff Nurse III, neonatal/pediatric nurse
Mt. Washington Pediatric Hospital
What does your job entail? I take care of neonates and infants with different diagnoses ranging from prematurity, drug withdrawal, and birth complications to congenital anomalies, to name a few.
How did you get into nursing? I was hospitalized when I was 7 and the nursing student who took care of me was very kind. I wanted to do the same when I grew up.
What’s unique about what you do? We routinely see infants with uncommon diagnoses that other neonatal nurses may see once or twice in a lifetime. We also have patients for much longer than other units—weeks to months—so the families become our families.
What do you consider the profession’s greatest rewards? Even if the outcome is a sad one, if you helped a parent cope with it, how can that not be the greatest reward?
Can you give an example of a time you felt especially rewarded by your job? I have watched a mother so scared to touch her infant because of all the tubes and equipment; she would just sit and stare. She would have to learn to care for the child with all the equipment at home (tracheostomy, ventilator, gastrostomy tube, etc.). I told her I knew she would be able to do it. She slowly learned with our encouragement. By the time they were discharged, the mother was telling us exactly how to do his care, how to suction, and how he liked his formula given. She was now his best advocate. It is the best feeling—to know you were a part of such growth.

Christina Purificato
Critical-care registered nurse
University of Maryland Medical Center
What exactly do you do? My official title is Clinical Nurse II, and I work in the surgical intensive care unit at University of Maryland Medical Center. I have worked in the SICU for the past two years, but have experience in the medical intensive care unit and cardiac surgery ICU, as well. The patients I care for suffer from various illnesses, ranging from bowel obstructions to end-stage liver disease requiring transplantation to ruptured aortic aneurysms.
What’s the most important attribute for a critical-care registered nurse?Flexibility. A patient’s status can change in the blink of an eye. I have watched a stable patient, sitting in a chair talking and joking with me about how young I look, and in the next breath, his eyes roll back in his head and his heart stops on the monitor. I have had days on the unit where I feel comfortable maintaining my two patient assignments only for a Code Blue to be called in the cardiac cath lab. Holding the code pager, I have to run into an unknown situation in an unknown corner of the hospital where someone is actively dying. The hat of an ICU nurse is always changing.
What is the profession’s greatest reward? Saving that patient. It is fascinating to me to watch the human body undergo an incredible amount of damage, only to heal, repair, and become strong again.
What would you be doing if you weren’t in this field? I would be a professional baker somewhere, making treats that are sugar-frosted, dipped in chocolate, and fried in lard.

Joseph Henry
Neonatal Intensive Care Unit
Greater Baltimore Medical Center
How did you get into nursing? In 1980, I started working at Mercy Medical Center as a temporary storeroom clerk in the lab, then as an attendant, mostly on the night shift. During those early years, it was typical that you were floated to multiple units, so I was able to learn how registered nurses worked. I especially was drawn to the encounters that RNs would have with the patients and their families, and decided nursing would be a great career choice for me.
What do you consider the profession’s greatest reward? The nursing profession affords us the honor to be with infants, parents, and families when they are most vulnerable. Making a difference to them is special and allows a closeness that is humbling as their trust in us grows.
Can you give an example of a time you felt especially rewarded by your job? One special event was when I was asked by a family to attend the blessing of their infant in church. I think back to when he was born and all of the challenges that he and his family endured. When I was at the blessing, I reflected on my job and how wonderful it is that I can be part of supporting the family as they start to assume their role as parents of a NICU infant.
What advice do you give to new nurses? First off, I recommend new nurses try multiple clinical areas before making a decision to commit to one nursing specialty. Every unit or specialty has hidden gifts that you might not discover until you’ve experienced working there.

Harriett Knight
Psychiatric nurse
Lifebridge Health Sinai Hospital
How did you get into nursing? I originally wanted to be a biologist because I love science, but I changed my mind after graduating from high school. It was during the Vietnam War, and a lot of my friends were in the military, including some as medics or nurses, and I thought nursing would be interesting, so I went back to school to be an RN.
What’s unique about what you do? I’m able to see people get better. Years ago, many mentally ill people were warehoused in state institutions for years, but with advances in medications, they can be stabilized and many can go back and function in society if they take their meds.
What is your greatest challenge? Maintaining patient safety, in the mental health unit in particular.
What advice do you give to new nurses? Make sure it’s what you really want, because it’s very demanding and, as a science, it’s not always easy. There’s always something new you must learn, from new medications and technology to new record-keeping software, patient privacy laws, and patient-safety protocols.
What would you have done as a career if you hadn’t been a nurse? I’m trained as a forensic nurse examiner and certified as a nurse educator, as well, so I think if it had not been biology, it would have been teaching. I’ve taught nursing at both the high school and college level.

Danielle Koceski
Senior Clinical Nurse
The Johns Hopkins University School
of Medicine Division of Gastroenterology
& Hepatology
How did you get into nursing? My grandmother is a nurse, so it’s in the genes. My decision to become a nurse was solidified when I was hospitalized as a teenager. My nurses were so kind, compassionate, and caring and were my advocates when I was too ill to speak for myself.
How has nursing evolved? Nursing has changed from white uniforms to blue scrubs, from manual blood pressure cuffs to machines, from paper charts to computerized charting. But the qualities of a nurse remain constant: Caring, patience, compassion, and professionalism are just a few of our qualities. We are the heart of health care.
Can you give an example of a time you felt especially rewarded by your job? Recently, a patient cut out all the sugars and sodas in their diet and started exercising because of a five-minute conversation I had with them on the phone. Making a small change can make a huge difference in someone’s life.
What advice do you give to new nurses? I started my career as a bedside hospital medical-surgical nurse. I tell any new grad that’s the best place to start to get a good foundation of experience and knowledge. The great thing about nursing is that there are so many opportunities and specializations, you can continue in nursing and change specialties. I’ve been a nurse for 17 years and have been a school nurse, office nurse, surgical nurse, endoscopy nurse, and hospital nurse, with many different specialties in all of those jobs.
The ListThe Envelope, Please!Here are the winners of our Excellence in Nursing survey, organized in 17 nursing specialties. Acute Care/Family Practice/General MedicineSusan PribylCharge nurse MedStar Franklin Square Medical Center Brigid Carey Intensive care, MICU The Johns Hopkins Hospital CardiovascularJoJo AbrenicaClinical leader LifeBridge Health Sinai Hospital Progressive Care Unit Theresa DeVeaux Acute care, vascular surgery University of Maryland Baltimore Washington Medical Center Chona Rizarri Cardiovascular surgery University of Maryland Medical Center Deborah Rouse Vascular access nurse MedStar Franklin Square Medical Center Donna Thompson Cardiopulmonary University of Maryland Upper Chesapeake Health Jackie Bradstock Cardiovascular The Johns Hopkins Hospital Community Care/Merrill Chaus |
Alphabet Soup
So, let’s take the case of our survey adviser, Joann Oliver. Her friends may know her as Joann, but, to you, she’s Joann M. Oliver, MNEd, RN, CNE, CBIS. Say what? To translate that, here’s our cheat sheet of just a few of the nurse certifications, degrees, and other stamps of approval, courtesy of Mt. Washington Pediatric Hospital human resources manager and RN Monica Atkinson.
ANCP-BC: Acute-Care Nurse Practitioner, Board-Certified.
BSN: Bachelor of Science in Nursing.
CBIS: Certified Brain Injury Specialist.
CCNS: Acute/Critical- Care Clinical Nurse Specialists.
CCRN: Acute/Critical- Care RN.
CEN: Certified Emergency Nurse.
CNE: Certified Nurse Educator.
DNP: Doctor of Nursing Practice.
LNHA: Licensed Nursing Home Administrator.
LPN: Licensed practical nurse.
LVN: Licensed Vocational Nurse.
MSN: Master of Science, Nursing.
MICU: Medical Intensive Care Unit.
MNEd: Master’s in Nursing Education.
NICU: Neonatal Intensive Care Unit.
NE-BC: Nurse Executive, Board-Certified.
NP: Nurse Practitioner.
Ph.D: You already know this one.
RN: You guessed it, again.
All in a Day's Work
For an ER nurse in the big city, there’s no such thing as a boring shift.
By Christianna McCausland

At 11 a.m. on a typical workday, Jessica Black, RN, clocks in for her 12-hour shift in Sinai Hospital’s Department of Emergency Medicine, known as ER-7. Like a football team huddling, all the nurses gather for shift report. It’s the moment they review any new policies and equipment, go over who’s covering which jobs—such as triage nurse or rapid-response nurse—and who will be the “float” nurse to cover everyone during their lunch hours. Black recalls one morning in particular, right after the shift report, when she was assigned four patients to cover.
On that day, everything started out pretty routine. Amongst her charges’ complaints were a toothache, a bellyache, and chest pain. Since she was always prioritizing, the chest pain was her first stop.
“I like to eyeball all my patients, even if I’m not doing a full assessment, and say, ‘I’ll be right back,’ then I’ll go to my sickest [patient] first,” says Black, who holds a Bachelor of Science degree in nursing and is a certified emergency nurse. The belly-pain patient, an older woman, was very insistent, so Black tried to make her comfortable before moving to the chest-pain case. She got the woman some Maalox. But Black’s seemingly uneventful day ended there.
“As she’s drinking it, it spills out of the left side of her mouth,” Black recalls. “So I ask her to try that again. Then I asked her to give me a smile and she’s only moving the right side and the left is drooping a little—she was literally having a stroke in front of my face.”
The team immediately delivered tPA, an intravenous medication that dissolves blood clots, and the woman stabilized nicely. But there was little time to celebrate. In a 56-bed emergency department that sees 200 to 250 patients a day, you never know what to expect. But that’s what turns Black on about her job. “I love not knowing what you’re going to get,” she says. “It keeps you busy and you’re always on your feet. I don’t like to sit.”
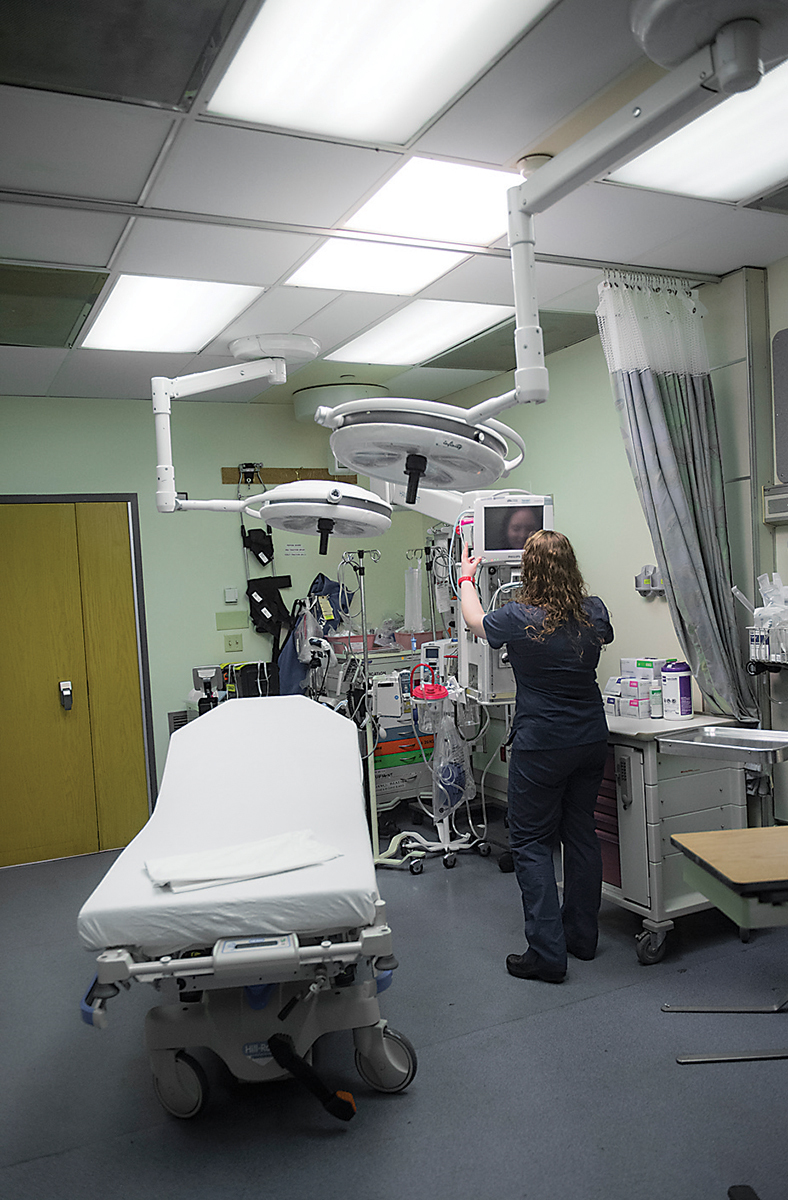
The 25-year-old Perry Hall resident joined Sinai right out of nursing school in 2012, attracted by the fact that Sinai is a level II trauma center, as well as a cardiovascular institute and stroke center. She was hungry to learn and knew a busy, urban emergency department was the place to do it.
As at most EDs, one common complaint at Sinai is chest pain, but on any given day, it’s not uncommon to have someone in cardiac arrest, a gunshot victim, or victims of car accidents. In addition to the trauma patients, Black also sees a lot of very sick people, like cancer patients with uncontrolled fevers and dialysis patients with fluid overload.
Then there are the seasonal outdoor injuries: If it’s spring, the ED might get the older men who didn’t get the memo about their age and fell off a ladder while cleaning gutters. In the winter, other weekend warriors return with heart attacks from shoveling snow. Kids’ sports injuries spike in the spring, as do motorcycle accidents. Late summer and fall? Think kids with football injuries.
But unlike the quiet suburban hospitals in Towson or Rosedale, Sinai is also the ambulance drivers’ frequent choice for shooting victims in that area of the city, and those cases are a pretty common occurrence for a hospital on the border of some of Northwest Baltimore’s poorest and most drug-ridden neighborhoods. They used to spike in the warm months, but recently Black has been seeing them regardless of the season.
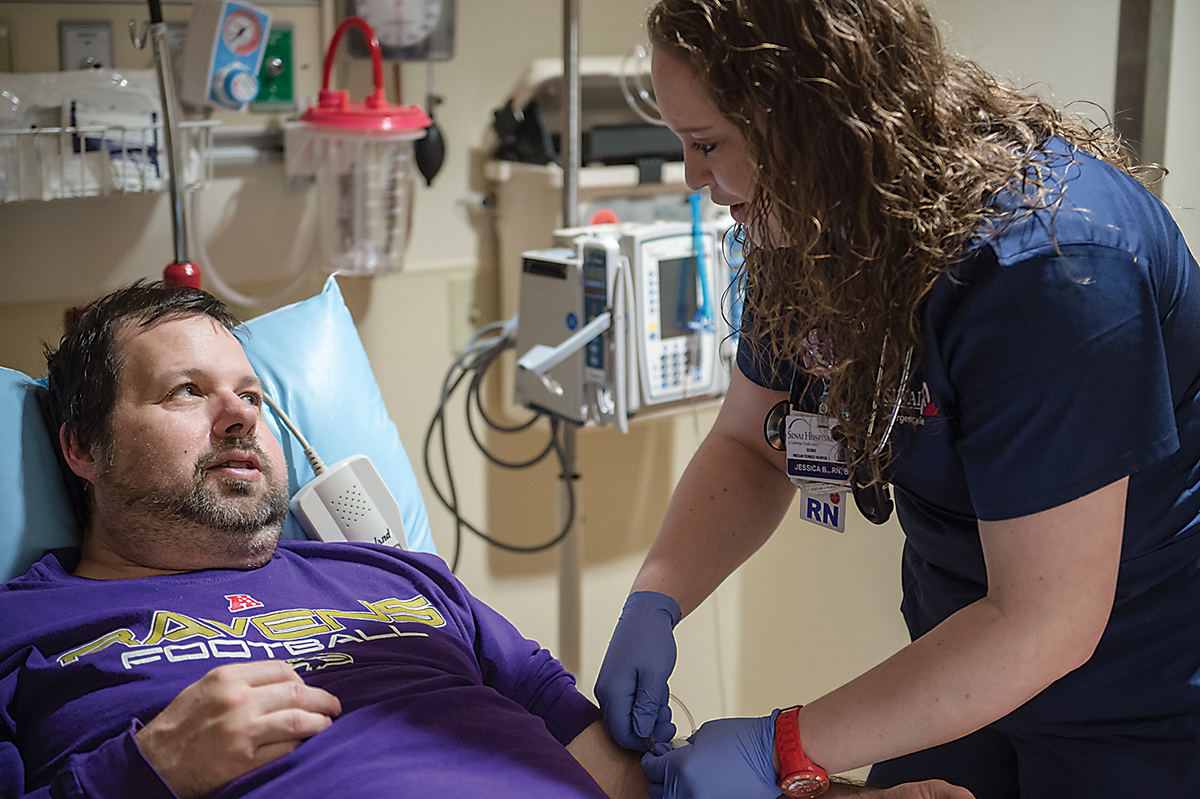
Despite the rush he gets from the trauma cases, Black also likes pediatrics. Sinai recently remodeled its pediatric emergency area, expanding it from eight to 13 beds. These little patients can be tough—Black has had medication spat in her face more than once—but they’re also a lot of fun. Until things go wrong.
“People tell you that you can’t cry, but any pediatric death is definitely very hard,” she says. “I’ve cried with patients and with mothers and fathers. There are times you tell them and they literally collapse in your arms. Those are the days when you get in the car and cry the whole way home.”
That’s the thing about emergency departments, or EDs: While plenty of people come for relatively minor things like the flu and pregnancy tests, many people are there for life-or-death reasons.
Black keeps a journal. When things go well, like the one day she was doing compressions on a cardiac-arrest patient who successfully stabilized, she logs that in her book. In that case, she was able to see the patient reconnected with his girlfriend. On days when things go badly, she pulls the journal out to remind herself it isn’t always awful. But she’ll also tell you that affirmative journal entries aren’t enough—her job is one that requires an emotional shell.
“That’s the thing with ED nurses, you have to build a wall up,” she says. “We’re still nice and you have compassion, but if you don’t build a wall, everything’s going to beat you up and you’ll be upset all the time. That’s one of the things I needed to learn as a new nurse.”
Ironically, this is also part of the ED’s appeal for Black. If she worked on a floor with the same patients day after day, she fears she would get too attached. In the ED, though, there’s always a patient going out and a new one coming in.
Sometimes she takes down the patients’ names and follows up to see how they fared after they left her care. “Other times, especially if I know it isn’t going to be good, you just want to forget.”
Black is lobbying the hospital administration for a bereavement room where family notifications can take place and where sensitive conversations can happen (like whether it’s best to transfer a patient to hospice care). It is the physician’s role to inform a family of a death, though often a nurse is there for support. Black is trying to institute a more team-based approach to notification where the doctor, nurse, a security guard, a patient advocate, and someone from pastoral care would all be involved. She believes that would be better for the families and safer for the staff.
“Everyone has different reactions—you never know how someone is going to react,” she says. “You may have to tell a family that someone is passed and they might cry with you or they may start punching walls.”
She also envisions the bereavement room as a place where staff can debrief after particularly challenging patients. “It’s so busy, we just go on to the next patient instead of being like, ‘You know, that kind of sucked and I want to talk about it with somebody,’” she says. “We should have a room where people from that cardiac arrest [team] can say, ‘You did a great job,’ a place to talk about the bad things, but also hear the good things. We need to give ourselves time to take a chill pill.”
One of Black’s least favorite assignments is triage. In a busy ED, people wait. And wait. And they can get downright verbally abusive.
“They don’t realize you could have someone literally dying next door, and here they’re getting upset because you aren’t spending enough time with them,” says Black. “It’s hard because you can’t explain why [you’re delayed] and you can’t please everyone. You have to remind yourself they’re having a problem, too, that they don’t know what’s going on next door.”
And then there are the addicts. While the proliferation of Narcan (an opiate antidote) may have helped manage the load of heroin overdoses outside the hospital, Black says they still have cases where someone ODs and their friends dump them outside the ED doors.
“The majority of the time, we’re able to give them Narcan and they’re better,” she says, “but you want to shake them and say, ‘Do you realize what you just did there? You literally just died for a second and we saved you.’ You realize you can’t be mad at them because they have a problem. And you want to get them help, but you can’t force people to get help.”
At the time the elderly woman had the stroke with Black watching, Black was at the end of her orientation, a fresh-faced new nurse. Now she trains new orientees. The hospital’s training keeps staff abreast of everything, from how to handle an active shooter in the building to how to put on a hazmat suit if, for example, there were a chemical spill or you have a patient with possible Ebola.
When she became an ED nurse, Black never realized how culturally literate she would need to become. She has learned ways to respectfully work with patients who can’t use their call button or sign their name because they’re observing the Jewish Sabbath. And then, when it’s time to call the morgue, there are different cultural customs about the disposal of a body.
She has also learned a little police work. In the case of trauma victims, the patient’s clothes are entirely removed. If the police are involved, the clothes are bagged for them and the patient is photographed. If the person dies, the room itself becomes a crime scene.
The emergency department is so relentlessly busy that Black carries a pen and paper with her to take notes on her patients, because it could be hours before she can sit down at a computer to do her charting.
The emergency department is so relentlessly busy that Black carries a pen and paper with her to take notes on her patients, because it could be hours before she can sit down at a computer to do her charting.
“I like the fast pace where you have a stroke or a heart attack and you have to work, work, work really fast,” she says. “Or the trauma where it could be a stab wound in the leg, it could be multiple gunshots to the chest, or a car accident. That’s the kind of stuff I like. It’s not nice to see, but I’m always learning.”
Wanted: |
|
Racetrack TriageIf there’s one thing Black encourages all new nurses to do, it’s to work the Preakness. With its close proximity to Pimlico Race Course, Sinai is ground zero for all race-day mishaps, and Black has worked the department during the event as well as being part of a team that sets up a tent at the track on race day. “I say [to new nurses], you have to see this and then you never have to work it again. But you need to see it,” she says with a laugh. “That’s probably one of the busiest days and you better come up ready for it. You still have sick people having heart attacks, but then you also have all the young kids from the Preakness that are lining the hallways with their puke buckets.” |
ER 411About 136 million people will visit one of America’s emergency rooms this year. Here are some facts about their visits: 85percent of patients have health insurance.40.2million visits are caused by injuries.58The average wait to be seen is about 58 minutes.Less than 3 percent of America’s $2.9 trillion health care tab in 2013 was spent in ERs. |







