COVID-19
Fever Dream
I had COVID-19. I wouldn’t wish it on my worst enemy.
I wake up with a fever of 102 in the middle of a global pandemic. The first thing I should do, of course, is get tested for coronavirus. Not just for me, but everyone I have been in contact with recently—my husband, son, parents, and co-workers—but this doesn’t happen. My initial symptoms are insignificant. A few days earlier, on March 13, my head felt warm and buzzy, but perhaps I’m being paranoid? Maryland has just closed schools and encouraged people to stay at home and to social distance, and my son and I take walks around the neighborhood with our dogs. By Sunday March 15, I feel strange, but not terrible. I suspect a fever but none of our thermometers are working, so my husband orders batteries from Amazon, because there are no thermometers in stock at any of the drugstores near my house. I spend an hour combing through our bathroom closet, throwing away dozens of expired medications.
On Monday, the batteries have arrived. I officially have a fever of 102. I shiver, sweat, and ache in every bone and joint. I have no appetite, no sense of taste or smell. I am so tired I stay in bed all day. The only escape from this misery is sleep. I call my primary care physician who asks if I have been out of the country within two weeks (I haven’t) and if I have come into contact with anyone who had tested positive (nope). He asks if I have a sore throat, cough, or shortness of breath, then the primary symptoms of coronavirus besides a high fever. (I do not.) I ask if I can get a COVID-19 test and am shocked to learn that I do not qualify.
In the middle of an exponentially expanding outbreak, when thousands are dying daily, and the only tool we have to track and contain this virus is a test, a person with a 102-degree fever does not qualify? What kind of absurd, dark comedy am I living in? My doctor’s instructions are to stay home, hydrate, take Tylenol for the fever, and rest. He says to call him if my current symptoms worsen, or if I develop respiratory issues.
My husband moves into the guest room and forces me to drink Pedialyte several times a day, which is disgusting, but I can’t taste it anyway. I sleep for several days, rarely getting up, and when I’m awake, I read articles about the virus and our government’s lack of a coherent response that infuriate and terrify me. I think I’m getting worse, I tell my husband. He tells me to stop reading the news.
I didn’t know then that COVID-19 symptoms fluctuate wildly, that there will be periods where I feel almost normal and want to eat actual food or spend time out of bed, potentially infecting my family. Over and over I think, finally, the worst is over, only to have the fever return.
My husband and son have no symptoms, so we assume that I have the regular flu, an unfortunate coincidence, since both of them had gotten flu shots and I didn’t. After a nasty few days, it seems I am on the mend. On Wednesday, March 18, I read a novel and watch a movie with my family, sitting a few feet away from them. But that night, I feel a pinching in my lungs, a dry cough when I try to inhale, as if someone had tightened a belt around my chest. I can’t take a full breath.
I wake up at 3 a.m. with a stabbing pain in the left side of my chest. Is it my heart? Are my lungs collapsing? I can feel the steam rolling off me, and I’m lying in a puddle of sweat. I lie in bed for a while longer, wondering if I’m dying from COVID-19, and worse, if I have infected the people I love. At this point, it is just the beginning, but I don’t realize that yet.
Thursday morning, I receive a flurry of texts from friends and colleagues. Am I better yet? How am I doing? Have I gotten tested? Have I talked to my doctor? Have I seen the latest idiotic thing our president has said? Do I still have a fever? It feels like a personal failure to tell all of them that, no, I am not better, and yes, I still have a fever.
“I wake up at 3 a.m. with a stabbing pain in the left side of my chest.”
I call my doctor that morning, the minute his office opens. My sickness has gone respiratory, I tell him, thinking that now I will finally be tested. I have shortness of breath and a cough, in addition to the fever, which shoots up every time the Tylenol wears off. I am so weak, so tired, and in so much pain. I am shocked to find out that I still do not qualify.
On Sunday, March 22, eight full days since I first fell ill, I awake to a splitting headache coupled with new dizziness. Am I getting worse? Or is my body just overtired from fighting this thing? My doctor’s office is closed, so I leave a message. I’m surprised to get a call back that afternoon. He is clear and decisive. It’s time to go immediately to the emergency room.
It has been a week since I last left my house, a week since I’ve driven my car. St. Joseph Medical Center is the closest hospital to me, and when I get there, the ER parking lot is surprisingly empty. I park, hop out, and almost turn back after reading the sign in the window: “At this time, we do not have COVID-19 testing available for all patients.” There is a sad looking plastic tent and some caution tape in front of the main entrance. I enter through a side door, pressing the button with my elbow, trying not to touch anything.
Inside, there are two receptionists wearing masks and zero patients in the waiting room. “My doctor told me to come,” I wheeze from behind my mask. “He wants me to get a chest X-ray for pneumonia.”
Behind closed doors, they quickly identify me as a COVID-19 risk and everyone who visits me is encased in plastic masks and garments. They take vials of my blood and photos of my lungs. Within a few minutes, the ER doctor is telling me I have pneumonia, a common effect of COVID-19. He says my lungs look “very bad.” He says I am midway between the early and late stages of coronavirus symptoms, with the latter being a total collapse of the lungs. He wants to aggressively treat me with IV antibiotics, Azithromycin, for viral pneumonia, and asks if I want to be part of a clinical trial for use of Plaquenil, aka hydroxychloriquine, an anti-malaria drug that may or may not help but the president is touting as “very promising” on the news. At this point, I’ll take anything, although studies now show that the drug has made coronavirus patients worse and, in some cases, caused permanent heart damage.
The doctor wants to test me for COVID-19, but he is only allowed to if I fail two other tests first, so we begin. After 45 minutes, my flu test is negative. An hour later, my viral panel is negative, too. They then give me the COVID-19 test and tell me I should have the results in 48 hours. The doctor wants to admit me to the hospital.
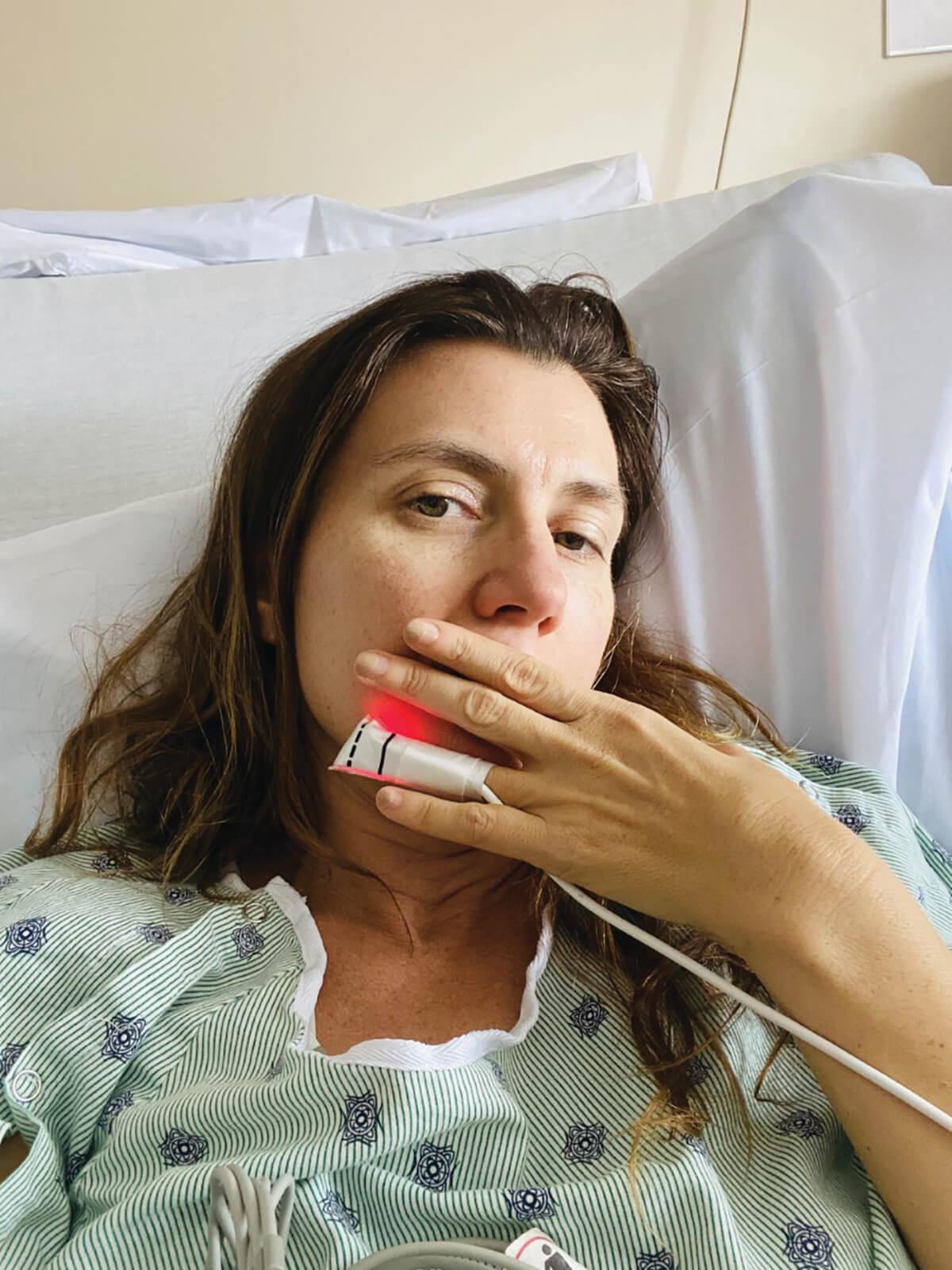

Cara Ober spent a lot of time in bed, separated from her family. Her dog, Mr. Big, was her sole source of companionship. -Courtesy of Cara Ober
My room is clean and quiet, and I appreciate the rest. It’s a comfort to know that professionals are monitoring my heart and lungs and I’m not going to die alone in the middle of the night.
A respiratory specialist visits me four times a day to administer an inhaler and test my lung functioning. A doctor visits once a day; I have no idea what his face looks like, but he gives me his cell number. He texts me from Eddie’s the next day and offers to bring me snacks, which is endearing beyond any normal scale of bedside manner. I have nurses who are so kind and generous that it brings me to tears. I realize they are risking their lives every time they enter the room.
After three days, my breathing begins to improve, and my doctor and I discuss an exit strategy. I still have not received my test results. He tells me I am potentially contagious for two weeks after my last fever and instructs me to behave as though I have been confirmed positive no matter what.
On Wednesday, March 25, I am discharged from the hospital. It’s cold and drizzly and surreal as I walk to my car, still sitting in the ER parking lot, which is still mostly empty. I look forward to sleeping in my own bed, and my husband and I have hatched a plan for me to quarantine in our bedroom with the dog, and for him and my son to essentially live their lives as far away from me as they can in the same house for the next two weeks.
I am still exhausted and have no appetite. I am getting migraine-level headaches every afternoon, but I can inhale completely, with just a small amount of coughing and I have an Albuteral inhaler to help my lungs. My pneumonia is on the mend. This time, I know better than to expect a speedy recovery. COVID-19 lingers and changes, flickers away, and returns with unexpected force. It is brutal and almost calculating, and this fluctuation in symptoms and false sense of improvement encourages its spread.
“I have nurses who are so kind and generous that it brings me to tears.”
A week and a half later, on April 3, I get a phone call from my ER doctor. My results have finally been faxed in and my test is positive, confirming that I was indeed infected with COVID-19. He says I no longer need to be quarantined from my family, a great relief, but I still tire easily. My senses of taste and smell have returned and I can finally breathe deeply. I am thankful.
Weeks later, the entire planet is still under lockdown, gripped with dread and fear due to the wide spread of COVID-19. I want to feel like my old self, but I know that I do not. As is true of most of the negative impacts of COVID-19, my current health situation could have been avoided if we had made well-informed decisions from the start. I did not need to get this sick, the same way our country could have prevented an economic collapse.
American capitalism has trained us to think we have control over our own lives, to the point where even serious health issues are a mind-over-matter problem to be quickly solved, but the coronavirus pandemic has revealed this to be a complete fantasy. We are not in control and we are not prepared and the U.S. healthcare system—or industry, as it actually is here (there are shareholders and payoffs, are there not?)—is not set up to care for people when they need it the most.
I worry about how long this is going to last, not just the risk to life and health but also to our economy, our culture, to the world as we have known it. All we have right now are our decisions and the impact of these choices. I wish I had said no to the clinical trial of hydroxychloroquine in the hospital, but I was scared and sick and desperate.
We all need to make better decisions. We need to hold our leaders accountable. We need to make sure hospitals are properly funded and those who work at them are supported and protected. We need to offer all Americans healthcare, which is not tied to their workplace, because jobs disappear during a health crisis and this further destabilizes our collective way of life.
Until then, I’ll be walking my dog with my son again, slowly but surely, grateful for every breath of fresh air.
