Health & Wellness
Inside Shock Trauma
A look at life and death in the world’s most advanced emergency room.
Allie Gold remembers being in the golf cart. She doesn’t recall falling out. Having completed her sophomore exams at the Maret School in Washington, D.C., the 16-year-old spent Memorial Day weekend with a girlfriend’s family on Gibson Island. The girls weren’t drinking, weren’t horsing around. It was the middle of a lovely day and Allie just fell out somehow.
An emergency room physician, by the hands of fate, was playing golf nearby when Allie’s head hit the concrete and she let go a deafening scream.
“I was home alone and I got a call, fraught with such anxiety, from her girlfriend’s father,” says Allie’s mother, Carol Weissbrod, who immediately asked a friend to drive her to Baltimore. “I knew she was in trouble. He said it was ‘dire.’”
The emergency room physician did not send Allie to the nearest emergency room. He requested a Maryland State Police helicopter take her directly to the R Adams Cowley Shock Trauma Center at the University of Maryland Medical Center in Baltimore.
Weissbrod called Allie’s father, Norman Gold, who was sailing on the Chesapeake. He got ashore and found a ride to Baltimore.
Dr. Thomas Scalea, Shock Trauma’s physician-in-chief and the attending physician that day, first wondered why what sounded like a minor accident victim was being brought to Shock Trauma.
“It seemed silly initially, with such a little accident,” says Scalea. “But she ends up with a very a serious brain injury.”
Weissbrod and Gold both arrived at the trauma center just after their daughter.
“We didn’t see her for a long time when we arrived,” Weissbrod says. “I don’t know how long; my perception of time wouldn’t be accurate. I was as frightened as I’d ever been in my life, and it began to go from bad to worse.”
First, Scalea’s team assessed her for bleeding. Allie, in fact, had bleeding in the brain, requiring immediate surgery. However, her brain continued to swell. Soon, her systems began to breakdown. Her lungs shut down. She went into cardiac failure. A few days later, her kidneys would fail.
“This was when Dr. Scalea and his team became very strategic and began trying one thing after another to save her,” recounts Weissbrod, a psychologist by profession. “I was a very anxious parent and Dr. Scalea would come and say, ‘We have to do this’ or ‘We have to do this.’”
Scalea’s team performed a craniectomy, opening Allie’s skull to relieve pressure. They also sliced open her abdomen, a procedure known as a laparotomy, relieving pressure in her torso and thereby her skull as well. Both are highly unusual techniques for treating a brain injury, according to Scalea, performed at few trauma centers in the world.
“She was an unbelievably sick kid.” Scalea says. “She was still dying when we opened up her abdomen, stood her upright.”
Her mother adds a sentiment echoed by many patients and families who have come through the Cowley Shock Trauma Center. “I don’t think she would’ve lived if she’d been taken anywhere else,” she says.
Surviving on a heart-lung machine during surgery, receiving dialysis, and with filters inserted to manage potentially fatal blood clots, Allie stayed in a coma for 21 days. Another week passed before she could be moved out of the intensive care unit.
“They felt like she began to turn a corner after 10 days and they knew she’d survive,” Weissbrod says. “Of course, no one could tell us what she’d be like mentally and physically. Later, a cardiologist told us it would be at least a year before she would be anything like herself. ‘That’s okay,’ I thought.”
Fifty years ago, Dr. R Adams Cowley, a pioneer in open-heart surgery, developed the first clinical shock trauma unit in the country, putting together a small staff and equipment—including two, and later four, beds—at the University of Maryland Medical Center. It was known as the death lab, at first, until patients given up for dead began to survive. Cowley’s credited with coining the idea of “the golden hour,” or as Scalea, the driving force at Shock Trauma for the last 13 years, explains, “the concept that trauma is a time-related disease.”
Today, with innovative techniques like those saving Allie, plus cutting edge x-ray, CAT scan, and MRI technology, ongoing research projects, U.S. military partnerships, violence prevention efforts, and a structure and communication system that countries from China to Italy wish to emulate, Shock Trauma remains at the global forefront of trauma care. Recent hardware upgrades include the largest hyperbaric chamber in the country and a digital x-ray machine, known as Lodox, which scans the entire body in 13 seconds. Developed in South Africa to search miners for diamonds, it was reconfigured for medical purposes.
“I’d like to think that the people in Maryland know they have one of the greatest trauma centers in the world in their state,” says American Trauma Society executive director Harry Teter. “Absolutely every specialty in medical care can be found there 24/7 and they attract the finest doctors in the country. I think people in the trade, most people, would acknowledge it is the best.”
When the yellow, mounted phone rings in the second floor of Shock Trauma’s resuscitation unit, a half-second of silence follows. A nurse quickly walks over and answers, grabbing a marker. Clunky, with an old-fashioned cord, the phone seems out of place in this bunker of computers and state-of-the art medical bays, each capable of serving as an operating room. She jots down the facts from the scene in shorthand on an erasable wall chart nearby: MVC (motor vehicle crash); ETA 17/18 (17 minutes for the helicopter to reach the accident site, another 18 minutes to Shock Trauma’s roof); +LOC (loss of consciousness); L4/L5 (back fracture); T5 (spinal cord injury, possibly indicating paralysis). Gender and age get marked down, too.
Later, a paramedic radios the attending physician directly, seeking advice with the deteriorating patient and asking permission to deliver morphine.
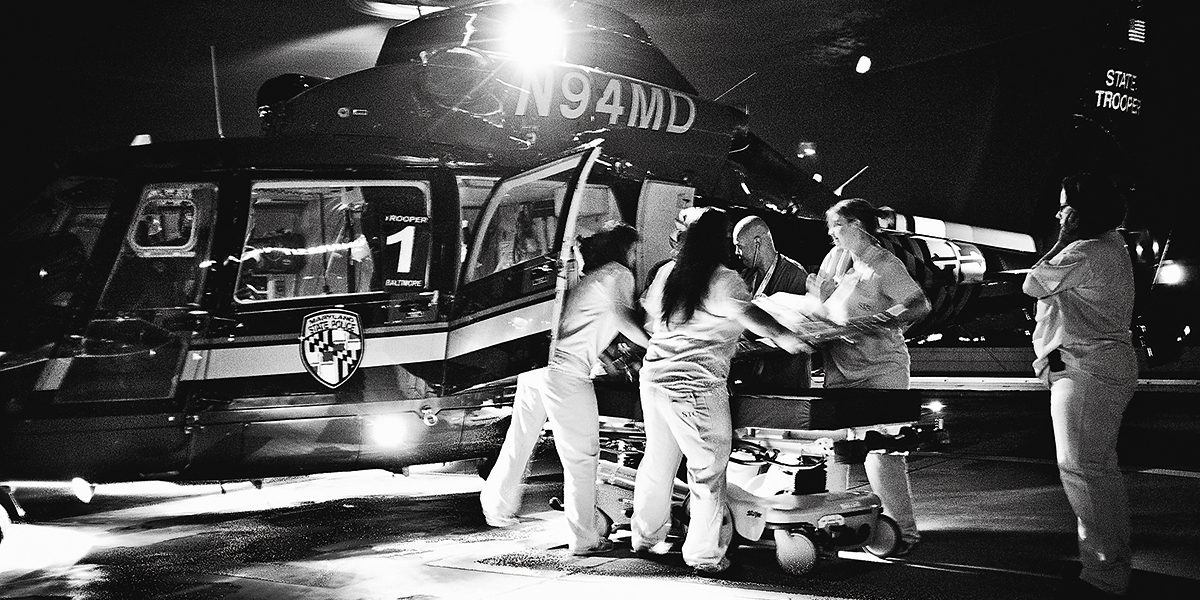
Then, minutes before the Maryland State Police helicopter arrives, two nurses take a dedicated elevator to the roof. At night, they spot it miles away, watching as a small light comes into view in the distance over M&T Bank stadium.
Not unexpectedly, the first wave of Labor Day weekend patients began arriving early Friday afternoon.
Just before 3 p.m., it was a middle-aged man, crushed by a tree. An hour later, a patient who’d fallen from a tree while intoxicated. About 90 minutes after that, a motorcyclist, found in the woods with a severed leg, was flown in—his leg alongside him in a cooler. The next minute, an unrestrained backseat passenger, she’d been ejected from an automobile after a crash.
Later, an elderly woman who’d fallen riding a bike. A minute after her, a young woman, pushed from a car. In the early evening, a pedestrian, struck by a tractor-trailer, landed on the helipad. By 10:45 p.m., 15 people had been admitted since mid-afternoon, including a victim with two bullet wounds to the neck. He died shortly after midnight.
By 5 p.m. the following day, another 24 patients arrived.
“We tend to get a lot at night, between 8 p.m. and 2 a.m.,” said nurse Meghan Brady. Like most of the nursing staff, Brady works three 12-hour shifts a week. The worst nights are pretty rough.
“I remember losing three in a row, right there in Area 4,” she says, gesturing behind her.
Cheri Carver, another nurse, has been at Shock Trauma for 15 years, raising eight children along the way. She’s treated neighbors’ children and saw a friend’s child die here. A big responsibility for nurses is taking care of patients’ families.
“Some families get it, understand what’s happening, and others don’t cope so well,” Carver says. “I have to give death notifications, and at least as far as it goes, I’d like to think I’m good at it. But you never know how to handle it. Some families are stoic, like if their kid sells drugs and they thought they might get this call someday. With others, and I’ve had to do it a lot, I’m praying with mom in the hallway.”
Early Saturday evening, a minor, shot in the face below his left eye, is wheeled into a bay, accompanied by police. Conscious, wide-eyed and scared, blood dripping from his wound, his chin and neck swelling with fluid, a dozen doctors, fellows, residents, nurses, and trauma techs surround his stretcher.
“He’s a baby,” someone says.
In a rehearsed choreography, a nurse cuts off his clothes as another asks for his parents’ phone number. An IV gets started. Blood pressure gets checked. Doctors look for exit wounds. Blood’s suctioned from his mouth. An anesthesiologist begins a sedative, preparing him for tracheal intubation. Blood gets drawn. Out of immediate danger, he’s readied for x-rays.
“I see where it is,” Dr. Deborah Stein says, minutes later, examining three-dimensional images on her computer and staring at the bullet lodged in the teenager’s lower neck. “But how did it get there?”
The three-day Labor Day weekend total was 107 admissions. Many were discharged within a day or so, but the 104-bed hospital remained at capacity. As usual.
U.S. trauma centers typically admit about 3,000 to 3,500 patients a year. Shock Trauma admits 8,000 annually. It’s the largest facility of its kind in the U.S. Ninety-seven percent of those patients survive.
“We each have very defined roles,” says Stein, at Shock Trauma since 2002. “As a result, I think, we are able to provide a really high level of care. What makes Shock Trauma stand out, however, she says, is having “the capacity to rev up and deal with whatever comes through the door. And you will never hear any grumbling from anyone.”
Ultimately, Labor Day was not dramatically different from other summer weekends. The hospital’s 13 Trauma Resuscitation Unit bays and 104 critical care beds regularly double up with patients. It’s a major reason for its $160 million expansion, which broke ground this spring. The new tower will add 64 ICU beds and 10 operating rooms.
Stein, like Scalea, acknowledges the pace and uncertain nature of Shock Trauma, while not for everyone, fits her personality—and is rewarding at the same time.
“I like not knowing what is going to happen every day,” she says. “But the other thing I love, too, is seeing people get better every day.”
Yet the workload and the tragedy, she admits, can be overwhelming at times. Doctors typically work 12- or 24-hour shifts to minimize handing off fragile patients.
“We struggle like much of the medical community to reduce hours for physicians while maintaining care,” Stein says. “But we are always prepared. We never say ‘no’ [to a request to bring a patient to Shock Trauma].” The policy comes directly from Scalea.
Since taking over as physician-in-chief in 1997, when Shock Trauma admitted 5,700 patients, Scalea has significantly expanded clinical services while also reorganizing research and education programs.
One of five children raised by a single mother in a large, “very Catholic” family in Rochester, N.Y., Scalea does not downplay that his work is his life—other than being known as a doting uncle among his staff.
He leads by example, performing some 600 operative procedures annually; 100-hour weeks are not unusual.
“I always wanted to be a musician, but I wasn’t good enough,” says Scalea, a trim, 59-year-old with a generally quiet, serious demeanor, albeit one that includes a dry sense of humor. He says his brothers and sisters are all very accomplished in a variety of challenging fields. “This is the only thing I am good at. When it’s 2 a.m. and I’m here, I feel confident I know what I’m doing.”
“I never got married and the truth is, the staff here is my family—and they know it,” he continues. “I know, for myself, I have never met a more committed group of people in my life.”
Among Shock Trauma’s unique partnerships is a collaboration with the University of Maryland School of Social Work’s Violence Intervention Program (VIP).
When a victim of gun violence, such as the above-mentioned teenaged survivor, comes into Shock Trauma, they’re visited within days by a caseworker, hoping the experience will provide them pause to reconsider their lifestyle.
“We refer to it as the second ‘Golden Hour,” says trauma surgeon Dr. Carnell Cooper, who founded VIP 12 years ago. A published 2006 study revealed participants were three times less likely to get arrested than non-participants; six times less likely to become a victim of gun violence again. It was one of the first hospital-based anti-violence programs in the country, and Cooper has since assisted other trauma centers in developing similar programs.
It’s an unfortunate coincidence, of course, but Baltimore’s level of gun violence—as well as the volume of crush and penetration victims handled at Shock Trauma—comes close to replicating the reality faced by military medical personnel. And so, on a different front, Shock Trauma partners with the Air Force’s Center for Sustainment of Trauma and Readiness Skills, training soon-to-be-deployed surgeons and medical personnel. Scalea, in fact, has flown with missions in Iraq and Kuwait, observing military procedures and protocols.
“Dr. Scalea and his staff are a phenomenal resource for us,” says Dr. David Powers, the deputy director of Shock Trauma’s C-STARS program that works with the Air Force. “Shock Trauma has an international reputation and in terms of our mission, battlefield medical care, evacuation, this is exactly what we see in their work with the Maryland State Troopers.”
Trooper First Class Eric Workman and Montgomery County police officer Alanna Ward knew Shock Trauma from their earliest days in law enforcement, but their first visits to the trauma center were as accident victims. Workman, who light-heartedly refers to himself as “a two-time alum,” returned as a gunshot victim.
Both reserve special praise for the individuals at Shock Trauma, and speak specifically of Scalea in near reverential terms.
In 1998, while working uniformed patrol, a negligent driver struck Workman from behind. Thrown 60 feet, he spent two weeks on life support, undergoing a dozen operations, and made a full recovery.
In December of 2006, Workman was shot while part of a team delivering a warrant in a pre-dawn raid. He spent two days on life support, undergoing three operations and the removal of his spleen. Scalea served as his primary physician both times.
“When I got shot, I knew I was hit bad, and I was telling somebody to call Shock Trauma and try to get Dr. Scalea—that’s what I’m preaching as I’m getting into the helicopter,” Workman recalls. “Sure enough, he’s there shortly after I arrive.”
While off-duty in 2007, a road-raging driver forced Alanna Ward off Interstate 270. Her husband, Michael, also a police officer, received a call from firefighters, who told him there had been a crash and his wife was trapped beneath her SUV.
Her vital signs started to crash as soon as she was pulled out and her heart stopped in the helicopter.
“They never got the heartbeat back in the helicopter,” she says. “I don’t know exactly how long I was dead before they got me to the trauma room and brought me back, but it was probably about six minutes.”
As in Allie Gold’s case, Scalea, who oversees all first responder cases, eventually opened Ward’s abdomen to relieve pressure in her brain. Ward still struggles with intestinal issues, but after three and half years, she’s planning to return to work this fall, initially in an administrative capacity.
Now 22, Allie struggles with similar intestinal issues linked to the abdominal surgery that saved her and Ward’s lives, but it’s improved with time and medication.
Also, like Ward, Allie intends a career in public service. Today, she’s a first-year student in Vanderbilt’s graduate nurse practitioner program.
“One of the things Shock Trauma did was allow my brother, who’d just graduated from medical school in New York, to go on rounds. He was kind of the translator for my parents,” Allie says. “I’m not sure everyone would do that.” She adds, however, it’s simple things, the bed baths and the changing of the linens, that patients remember as much as anything.
Allie and her mother have also met with new patients and their families, as part of Shock Trauma’s survivor network, offering encouragement that recovery is possible.
“What was notable to us was the investment of the nurses and doctors,” her mother says. “Dr. Scalea travels all over the world, but when he had to go away, he’d call in to check on her condition. When she finally woke up from her coma, we’d gone out to eat in Baltimore. One of the nurses called us on our cell phone right away. They were so invested, cared so much, it was incredible.”
Allie’s experience, which included years of rehab and follow-up meetings with Scalea, who remained her primary physician, proved transforming.
“They never stopped trying new things, they never gave up,” she says. “My parents put a lot of trust in them, and it was definitely not easy for my parents; it was all an incredible shock for them. It changed my perspective. It changed me.”
She’s held several research jobs while in school, but when making her career choice, she knew she wanted closer interaction with hospital patients.
“I know I’ll make a great nurse practitioner,” she says. “I know how it feels to be in that position. I know that feeling and the difference people make.”