Partner Content
Since its spread into the MidAtlantic many years ago, experts have established that Lyme disease is caused by an infection from a bacterium called Borrelia burgdorferi, usually transmitted by a deer tick bite. Roughly 20,000 cases of Lyme disease are reported in America annually, with some sufferers never seeming to recover, and others struggling to get physicians to continue prescribing antibiotics beyond what is accepted practice.
But things are changing, on both the medical and regulatory fronts. We talked to Lyme disease specialist Dr. Kalpana Shere-Wolfe M.D., assistant professor of medicine at the University of Maryland School of Medicine and director of the Lyme program at University of Maryland Medical Center, to learn more about the disease.
Can you tell us a bit about your background, and your interest in Lyme?
I am an internal medicine physician with specialization in infectious diseases, critical care, and integrative medicine. I became interested in Lyme because of the lack of care for patients with Post Treatment Lyme Disease Syndrome (PTLDS) or Chronic Lyme disease – those who do not improve with antibiotics. In particular, I incorporate Integrative Medicine modalities, like meditation and yoga, to improve a patient’s quality of life. We have the capacity for self-healing through good nutrition, rest/sleep, movement, and positive-mindset support recovery. Tools such as our breath, body, and mind can aid in that process.
With the summer tick season here, what are the signs and symptoms of Lyme disease, and how is it diagnosed?
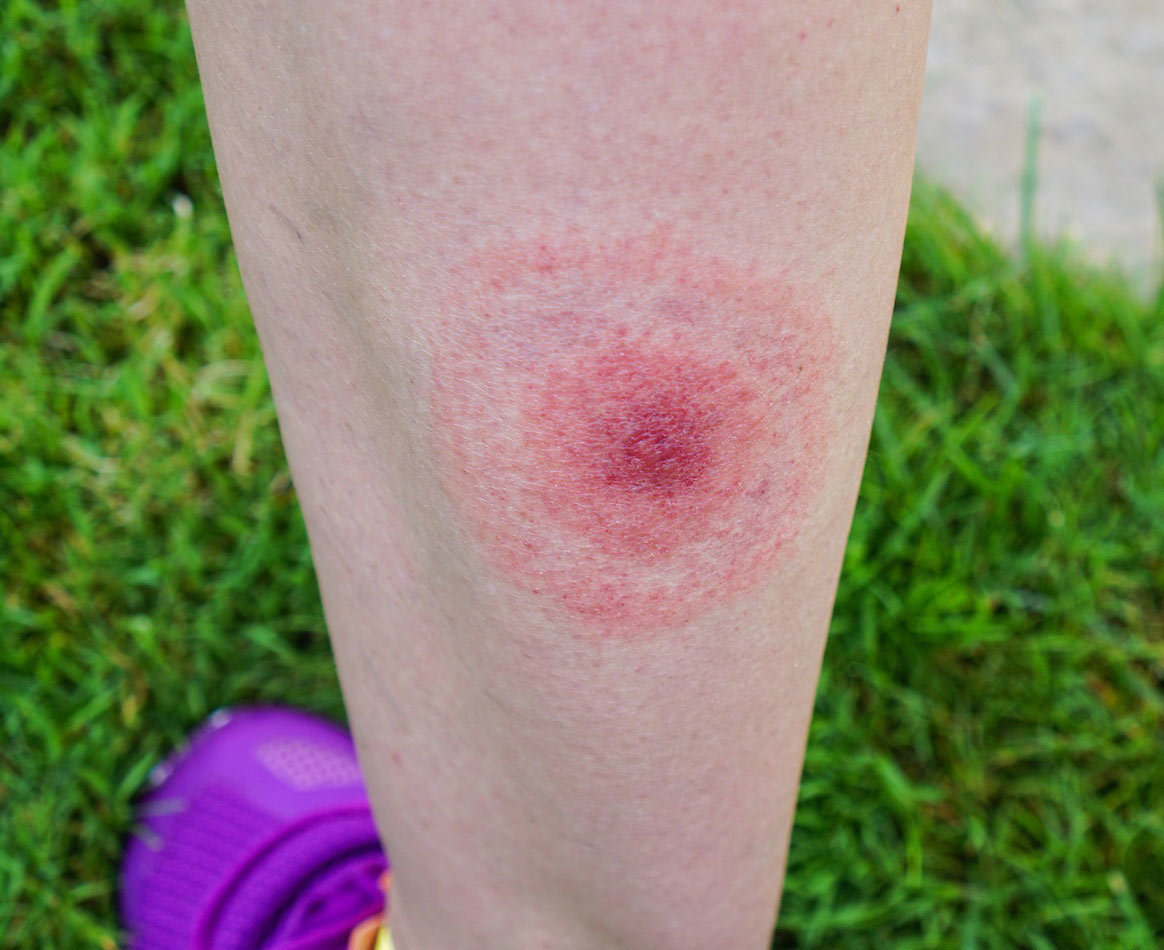
Early on, symptoms include fever, headache, fatigue, swollen glands, and possibly a bull’s-eye skin rash. But only about 70-80 percent of folks develop a rash.
In days to weeks after the bite, the infection may spread to the heart, nervous system, and joints. People may experience joint pains, stiff neck, enlarged spleen, sore throat, and irregular heart beat or palpitations. Months later, patients can experience intermittent attacks of joint swelling and pain, and possibly a subtle cognitive change.
Lyme diagnosis depends on symptoms, exposure, and history. Because the bacteria is difficult to culture, we rely on serology, a method of detecting antibodies. The CDC recommends two-tier testing: first an ELISA test, then a Western Blot test to measure the body’s antibody response. Typically when we have an infection, our body takes about four weeks to produce the IgM antibody. IgG are other antibodies which take longer to become detectable, making timely diagnosis challenging. Lab testing for Lyme disease can be confusing even for physicians, so it is important to remember that patients can be misdiagnosed as having Lyme disease.
What sorts of outdoor activities or conditions increase the chances of a bite from an infected deer tick?
Tick exposure is key. Deer ticks are found primarily in heavily wooded areas from Maine to Maryland and other western regions. Spending time in these areas with exposed skin increases tick bite risk.
How important is it to get quick treatment?
You should seek prompt medical evaluation if you are symptomatic or develop a rash, as Lyme disease can progress from early disease to disseminated infection, causing later, long-term issues. It’s also important to remember not every tick is a deer tick and not every deer tick is infected. If a tick is infected and removed early, the infection most likely won’t be transmitted.
Why do some patients never seem to recover?
Researchers don’t have an answer to this question. With any infection, people react differently with a range of symptoms. Variation in inoculum size (of bacteria), the severity of bacterial factors, and host immune response affect people differently.
In what ways has the liability of the medical profession changed regarding long-term antibiotic prescriptions?
Doctors are reluctant to prescribe long-term antibiotics without a clear need. Taking antibiotics long-term bears serious consequences and can cause antibiotic-resistant bacteria, a severe infection of the gastrointestinal tract, sepsis and septic shock, liver problems, and importantly, disruption and abnormality of gut microbiome – which is linked to obesity, diabetes, and inflammation. Trillions of bacteria of microbes live within us and are crucial to our immune function and well-being.
How has University of Maryland responded to the need for Lyme disease research and treatment?
In October 2017, we started an integrated Lyme program to provide care for patients with both acute and chronic symptoms. We treat Lyme disease with antibiotics when necessary. However, when symptoms persist, we start investigating other possible causes. Taking an Integrative Medicine approach, we focus on whole health, including natural health products, mind-body techniques, and other systems like Ayurveda and traditional Chinese medicine. We also focus on sleep, diet, movement, and stress management. Without sleep, fatigue, cognitive issues, and pain will not improve. Without a proper diet, inflammation and pain can become worse.


